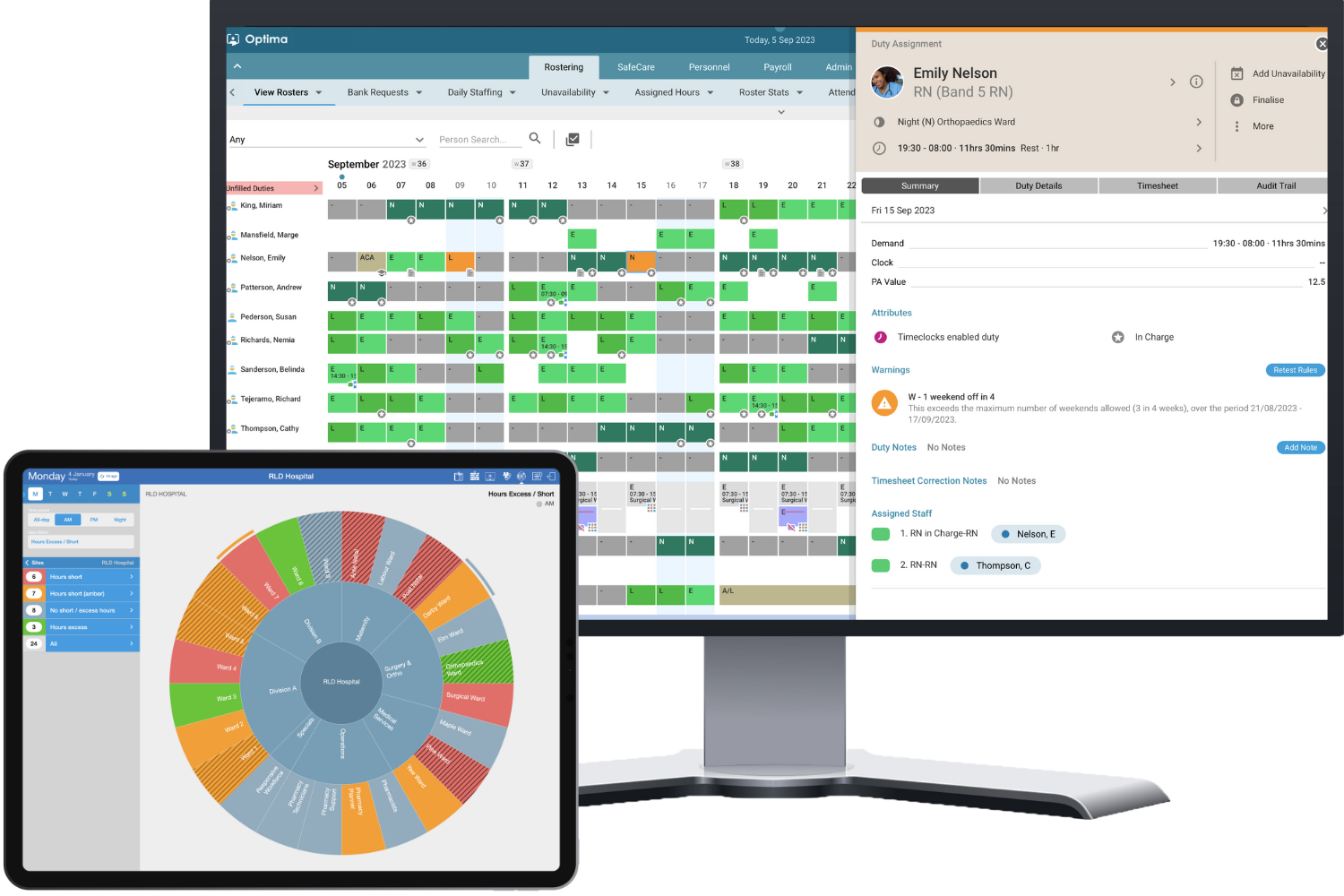
For us, workforce management is more than just creating a roster, and then revisiting it to run payroll. It’s about efficient use of your staffing resource you have available, so you can deliver a safe service.
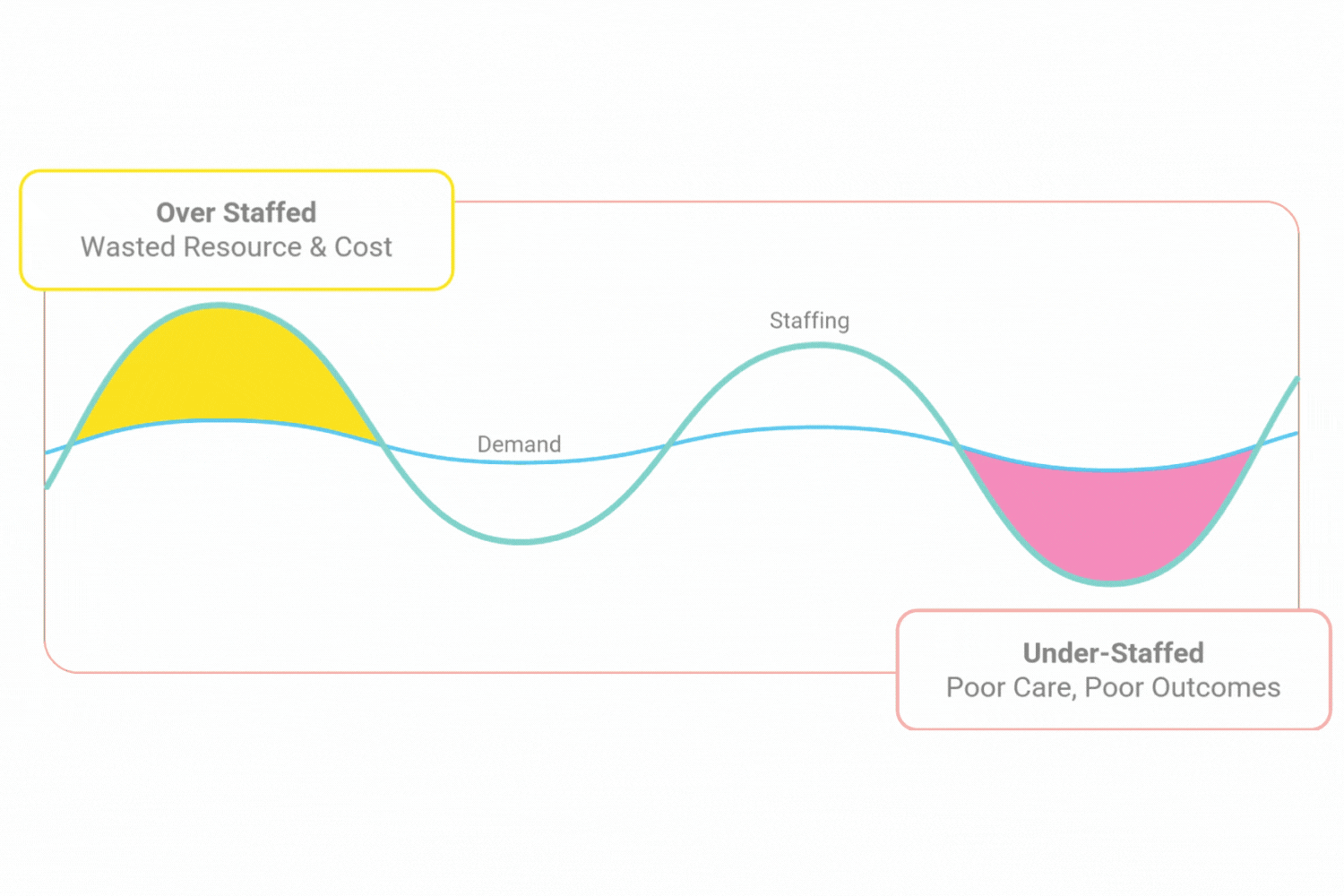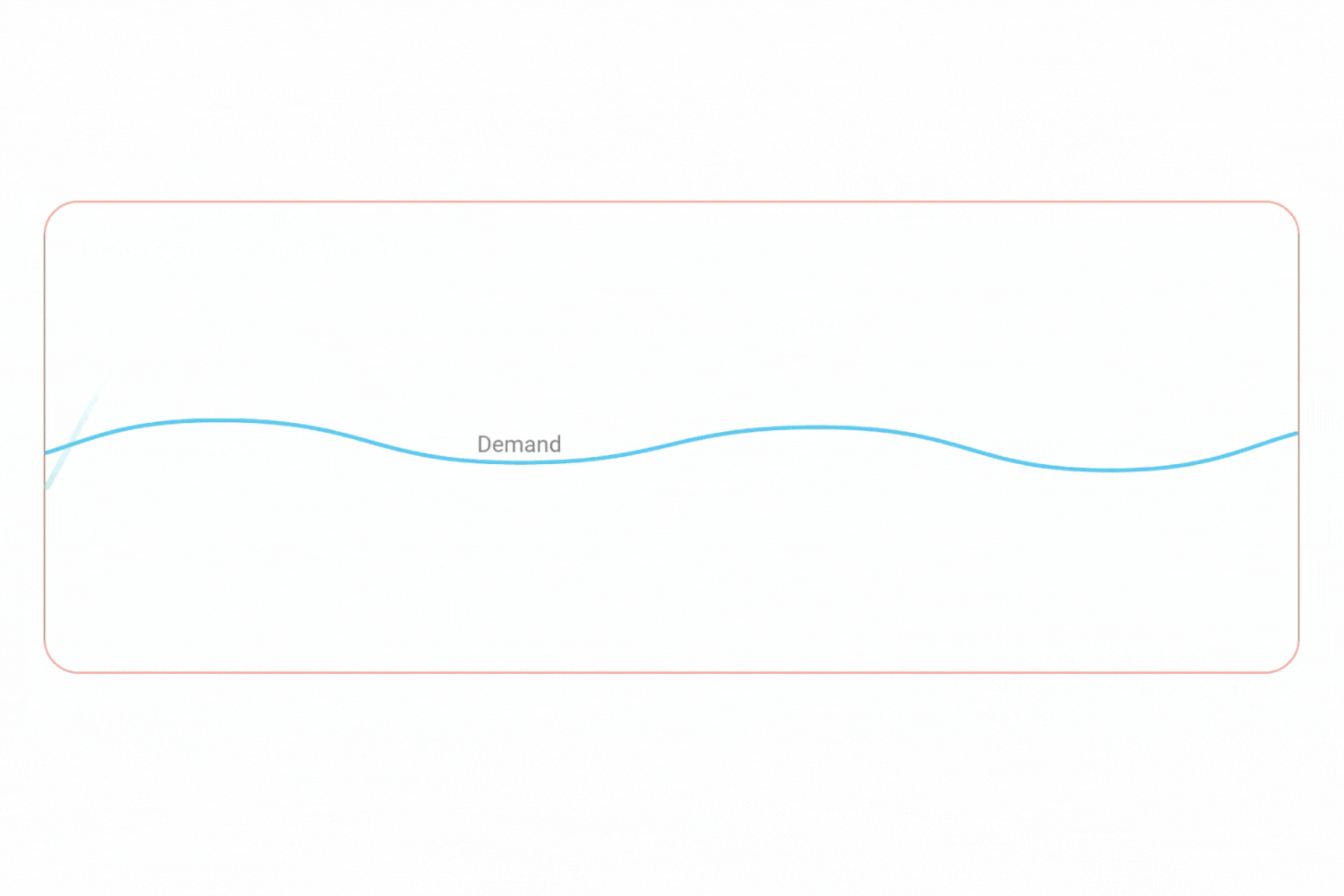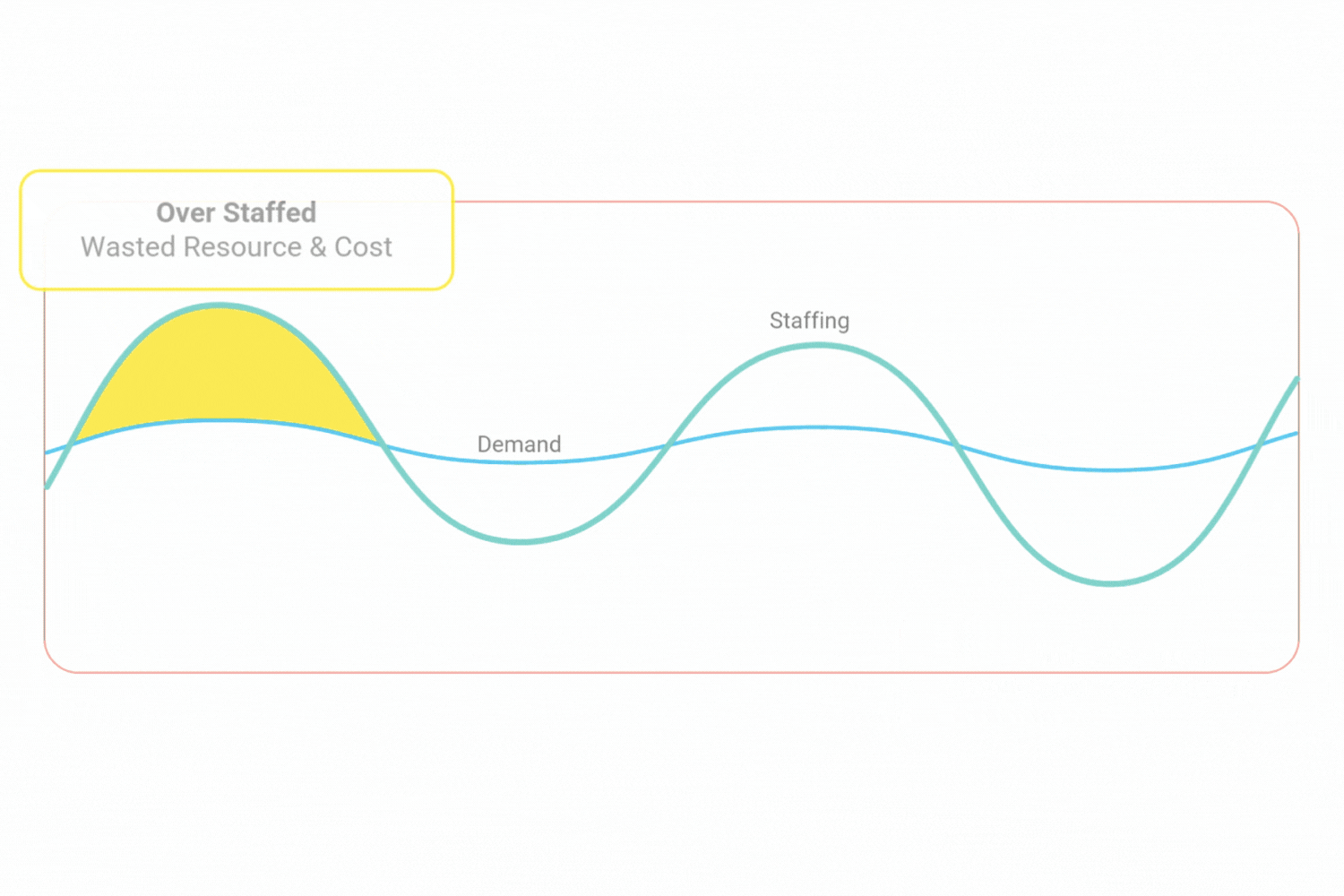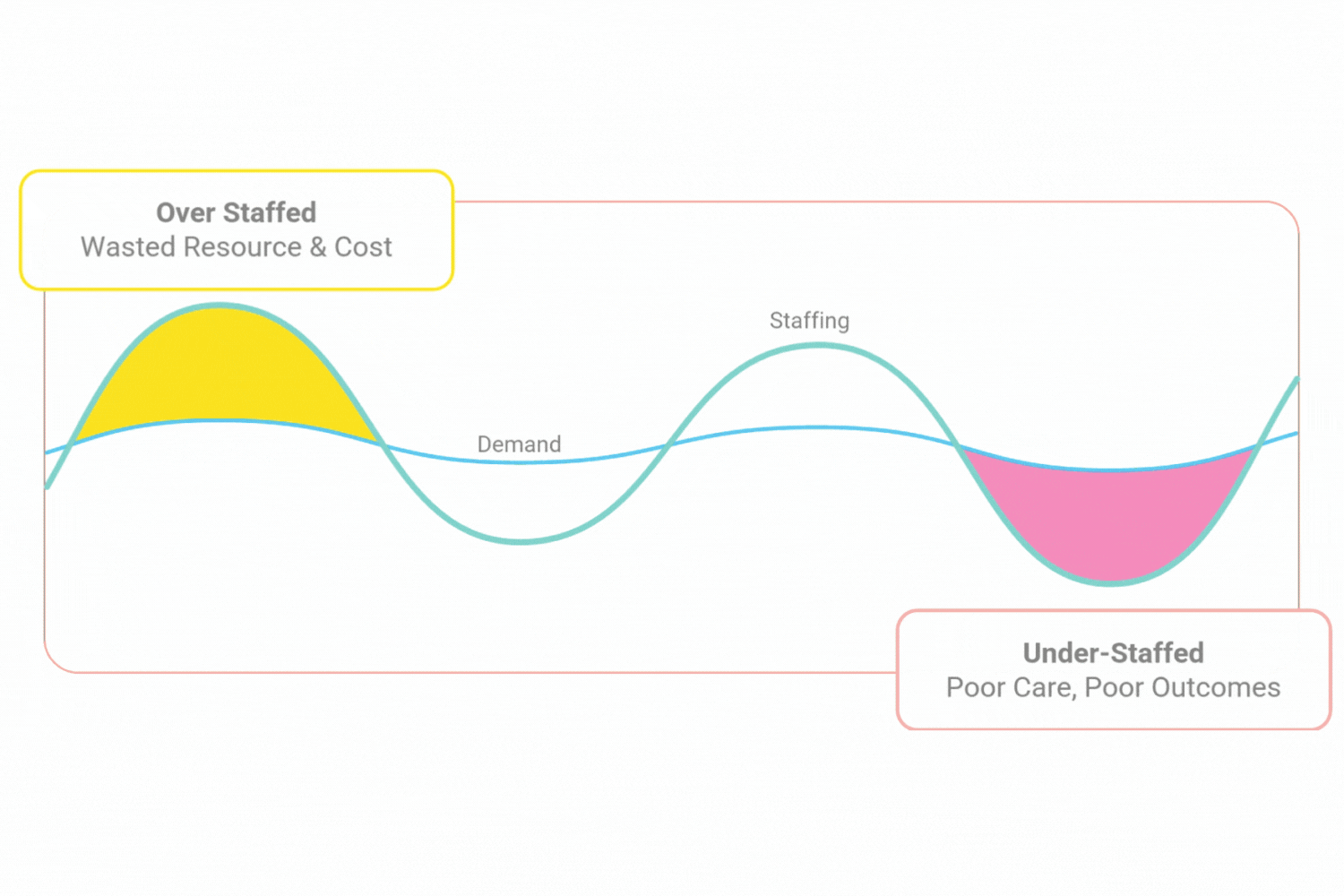
The old way leads to staffing gaps when there shouldn’t be and that are costly to fill, as well as times when you’re over staffed and wasted resource.
All this leads to unhappy, burnt out staff. Plus, an unsafe service for your patients & residents.